10 Sep Journey into Parenthood: Your Maternity Guide at Island Hospital
Journey into Parenthood: Your Maternity Guide at Island Hospital
By Island Hospital | Sep 10, 2021 5:45:27 PM
This is a simple guide to bring you through a journey from what to expect in a pregnancy, to giving birth and caring for your newborn. We will be delighted to accompany and share our know-how with you. Our aim is to ensure that your journey into parenthood is a unique experience that is both pleasant and enjoyable. We are committed to ensuring that you and your newborn receive personalised holistic care when you choose to deliver your child in Island Hospital.
1st trimester (until 12 weeks)
• Nausea with or without vomiting
• Increase urination
• Tiredness
• Food aversions
• Tender swollen breasts
2nd trimester (12 weeks to 28 weeks)
• Growing belly and breasts
• Skin changes
• Braxton Hicks contractions
• Leg cramps
• Vaginal discharge
3rd trimester (until delivery)
• Increase backache
• Frequent urination
• Heartburn and indigestion
• Shortness of breath
• Haemorrhoids
Are you all set for the big day? Here is a list of items to pack in you and your little one’s hospital bags to prepare for the big day. Once all the bags are packed, keep them handy, either in the car or near the door, so you will be ready to go at a moment’s notice.
MOM’S ESSENTIALS
A) Comfy Clothes and Foot Wear
You will need something comfortable to sleep in during your hospital stay
• Nightwear or Dressing Gown a soft, loose nightgown is a good option. Choose a front-opening style if you plan to breastfeed.
• Underwear Pack several pairs of comfortable underwear that are large enough to wear over heavy-duty maternity pads.
• Socks
• Anti-slip Sandals You will want sandals that are comfortable and easy to slip in and out
• Extra outfit to wear home Choose something loose-fitting, with a drawstring or elastic waist
Also, if you plan on breastfeeding:
• Loose shirts
• Maternity/nursing bra is a must.
• Nursing pads
B) Personal Care Items
You will spend a few nights in the hospital, so you will feel better if you have things that will help you “freshen up”.
• Toothbrush and toothpaste
• Bath and facial towels
• Soap
• Hair brush or comb
• Wet wipes
• Facial Tissues
• Maternity “stick on” sanitary pad
• Skin care products If makeup is part of your usual routine, then do not forget your cosmetics for those Facebook or Instagram moments!
• Glasses & contact solution if you wear contacts
C) Documents
• IC and also your partner’s
• Marriage Certificate (for registration of birth certificate within 14 days of delivery)
BABY’S ESSENTIALS
A) Going Home
• Bring newborn and 3-month sized clothes if you are not sure how big your baby will be.
• Blanket
• Socks, mittens and booties
• Swaddle
At Island Hospital, we strive for continuity of care from early to advanced pregnancy, during delivery and in the postnatal period. Where possible, the same qualified midwives who attend to your antenatal needs will care for you and your baby until the end of your hospital stay. Our midwives work in partnership with your obstetrician during the delivery of your baby to help make your birthing experience a pleasant and memorable one.
During Labour – Delivery Care
An experienced and qualified midwife will support you throughout the period of active labour. Your husband, if you wish him to be present, will be guided to give you support and comfort during labour.
Post Natal – Post Natal Care
You may have to stay in hospital usually for three days following a vaginal delivery and four days following a Caesarean section or as advised by your obstetrician. During this period, we will show you how to breastfeed and bath your baby. You will both be cared for and closely monitored in a conducive environment.
Birth certificates are issued by the National Registration Department (Jabatan Pendaftaran Negara) at its local branches. To register your child’s birth, you will be given the JPN LM01 form to fill. Our clerical staff will assist you and your husband in completing this form and direct you to the local JPN office. Birth registration must be done within 60 days of birth.
We are led by Obstetricians, Gynaecologists and Paediatricians while being supported by experienced midwives and post basic trained nurses. Multidisciplinary support is available at any time as to ensure mother and child safety.
Once you are registered with your obstetrician during early pregnancy, you have the option of attending our antenatal classes which provide information on pregnancy and parenthood, to prepare you for the birth and care of your newborn. Your husband is encouraged to attend these classes with you.
Single Room

Semi Private Room
We encourage you to proceed to the hospital:
• If your contractions are occurring at regular intervals or are causing you discomfort or distress.
• If you are losing blood from the vagina.
• When your waters break, whether you are having contractions or not.
When in doubt, it is advisable to telephone your doctor or our nurse at the hospital’s Accident & Emergency for advice.
If your labour commences and you do not have transport, please call for the hospital’s ambulance.
Ambulance/Emergency Services: 04-226 8527
Please leave all valuables at home.
12:00 noon – 2:00pm
6:00pm – 8:00pm
Getting optimum rest is paramount to every mother who has just given birth. Therefore, please request that your relatives and friends visit during visiting hours. This is to allow you to have as much rest as possible after delivery.
If you had a baby before, you will know what to expect. However, if this is your first child, it is important that you learn more about going into labour.
Labour is divided into three stages:
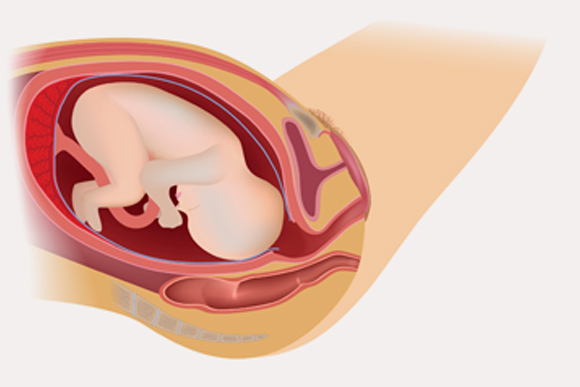
Stage 1
Cervix is fully dilated
This involves the dilatation or stretching of the cervix (neck of the womb). This stage may begin in any of the following ways:a) Womb contractions which may be weak at first but will gradually increase in strength and frequency.b) A small discharge of blood-stained mucus from the vagina – a “show”c) Leak of liquor (water surrounding the foetus)
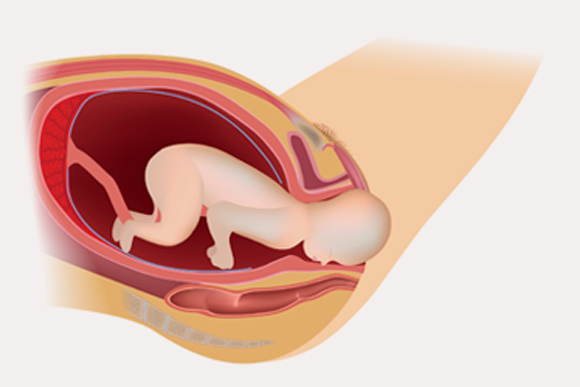
Stage 2
Baby’s head descendsThis starts when the cervix is fully dilated and the baby makes its way down, and out of the birth canal. The baby is born at the end of the second stage.
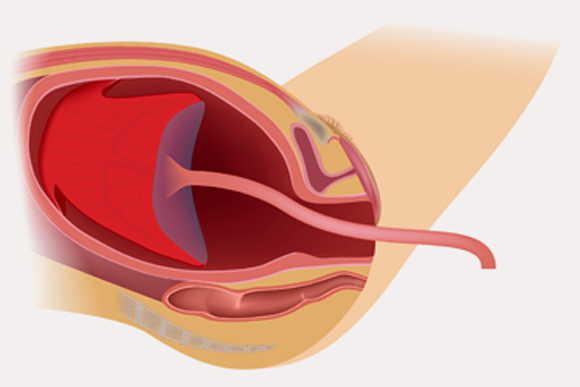
Stage 3
Placenta is delivered by doctor
This occurs shortly after the birth of the baby and continues until the expulsion of the placenta (also known as the “afterbirth”), is completed.
You may experience some labour pain during the delivery process. As an option, you may request for pain relief such as:
Diversional Therapy
• Aromatherapy (you may bring your own)
• Music (you may bring your own)
• Hot shower
• Gym ball (provided)
Entonox Inhalation
• Entonox (gas and air) is a colourless, odourless gas made up of 50% oxygen and 50% nitrous oxide. It’s also known as laughing gas. It can take the edge off labour pain, rather than blocking it out.
• Works well if instructions are followed.
• Available immediately upon request
Injection
• Injections of Opioid drugs are widely used for pain relief in labour,
• Relieves 40% – 50% of pain.
• May cause you to feel sedated.
• Available immediately upon request.
Epidural
• An epidural is a procedure that injects a local anaesthetic into the space around the spinal nerves in your lower back.
• Relieves 60% – 70% of pain.
• Done by an anaesthetist.
• You will need to get into a C-shape position for needle insertion.
• It may take an hour to have the optimum effect.
Before going home, your baby will receive two immunisation jabs – BCG and Hepatitis B vaccination. Your baby’s paediatricians will arrange to complete the rest of the required immunisation for your baby as stipulated in the immunisation schedule.
The World Health Organization (WHO) recommends all mothers to breastfeed their babies exclusively from birth until 2 years old, complimentary food (solid) should start at 6 months old.
You are encouraged to breastfeed your newborn as it will benefit both mother and baby. As a start, our experienced midwives will assist and support you throughout your stay in hospital. Feel free to ask for a copy of our breastfeeding booklet to aid you.
Benefits of breastfeeding:
• Promotes mother and child bonding.
• It helps to contract uterus and prevent uterine bleeding after delivery.
• Reduces the risk of breast and ovarian cancer.
• Helps mother to lose weight and get back to pre-pregnancy weight.
• A natural form of family planning (not absolute though).
Benefits to Child
• Breast milk has the most complete nutrition for baby.
Colostrum, mother’s first milk contains antibodies and is the baby’s first immunisation against bacteria and viruses.
• It reduces the incidences of cough, colds, ear infections, bronchitis, pneumonia and meningitis.
• Breastfeeding prevents colic and lowers the risk of gastrointestinal infections and diarrhoea.
• Breastfeeding protects baby from asthma, eczema, colds and food allergies.
Breastfeeding lowers the risk of baby developing juvenile diabetes and heart disease.
• It enhances baby’s IQ level.
This is an optional screening and is done only upon request by parents.
What is a Newborn Hearing Screening test?
Hearing screening programmes are developed to identify newborns with hearing loss so that timely treatment and rehabilitative measures can be instituted early.
Why is it important for my baby to have a Hearing Screening Test?
Significant hearing loss in both ears occurs in 0.1 to 0.3% of the well-baby nursery population, and 0.2% to 0.4% in the intensive care unit population. Another 0.3% will acquire hearing impairment in early childhood.
Hearing impairment can hinder development of the child’s communication skills, that is speech and language acquisition, which in turn can lead to learning problems.
How is the Hearing Screening Test performed?
The newborn hearing screening test will be performed in the nursery on infants within the first few days after birth, prior to the discharge of your child. The hearing test will be done by trained staff using Otoacoustic Emissions (OAE).
The OAE screening is safe and completely painless. Special probes are placed in the baby’s ear to generate and pick up signals presented to the ear.
Multiple test signals are averaged out and the result is read as “pass” or “refer to a doctor” for further evaluation.
You will get the results of the hearing screening test before you leave the hospital.
The following is a quick checklist when you are preparing to go home with your baby:
• Has transport home been arranged?
• Have you handed over going home clothes for your baby to the nurse in the Nursery?
• Have you received your baby’s Birth Certification from Island Hospital and the JPN LM01 form?
• Have you been advised on the clearance of hospitalisation fees and charges by the ward
receptionist or the ward staff?
• Have you collected your take home medicines from the Pharmacy?
• Have you received immunisation and KKIA booklet from the Nursery?
When you are certain that you have completed the above, you can proceed to the Nursery to receive your baby from the nurse in charge.