Home
Specialised &
Equipped
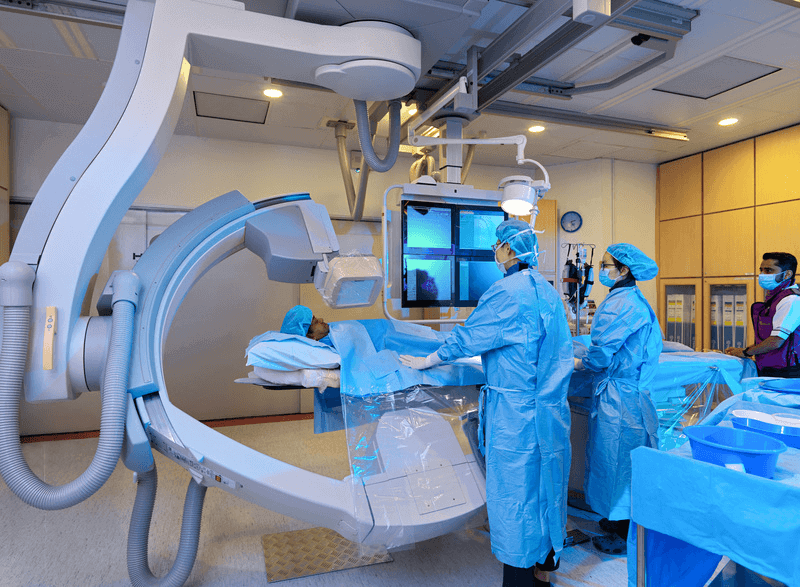
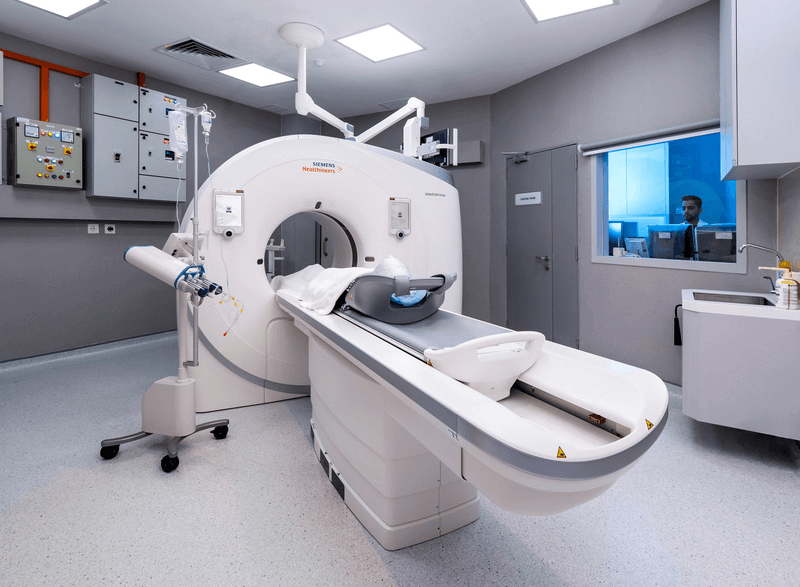
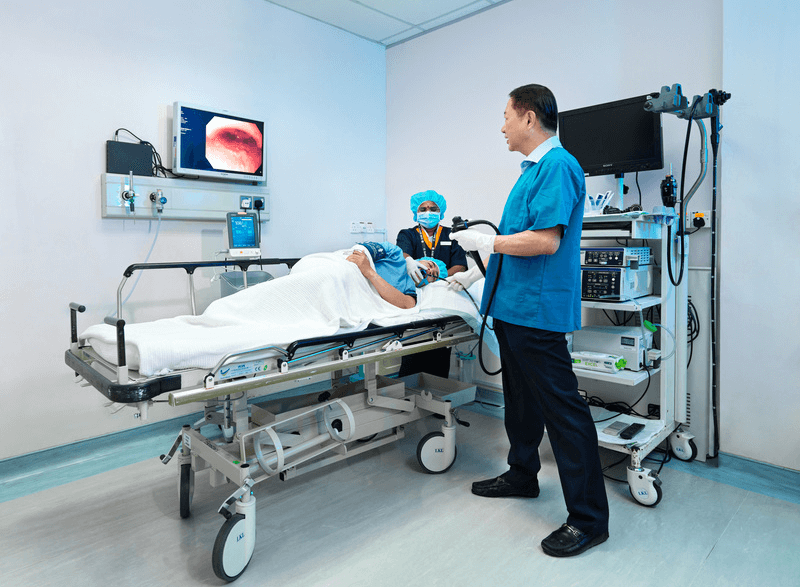
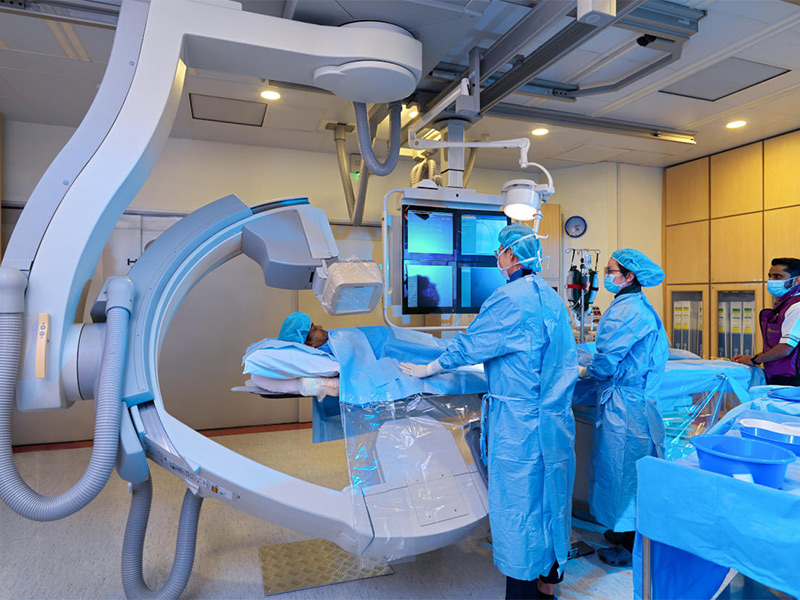
At Island Hospital, patients have access to some of the most highly respected specialists in Malaysia.
Packages & Promotions
Address
308, Macalister Road,
10450 George Town,
Penang, Malaysia
Contact
Information and appointment
+604 238 3388
24-hour Emergency Hotline
+604 226 8527
Toll-free in Malaysia
1300 880 788
Toll-free in Indonesia
007 803 601 5248
International Patient Service
+604-228 8222
Show
Map
×