22 Feb Why Hemorrhoids Happen, Its Common Causes, and How to Break the Cycle
Hemorrhoids: treatment, symptoms, causes
By Island Hospital | Feb 24, 2022 4:53:17 PM
Hemorrhoids, also called piles, are a common problem in Malaysia. It is estimated that three out of four adults will have hemorrhoids at some point of their lives. Hemorrhoids have a number of causes, but often the cause is unknown.
Fortunately, hemorrhoids are not life-threatening and there are effective options to treat the condition. Home treatments and lifestyle changes such as eating more fiber in your diet can manage the problem but if your hemorrhoids have not resolved within a week, it is best to see a doctor. At Island Hospital, you may consult any of our specialists for hemorrhoids treatment.
What Are Hemorrhoids?
Hemorrhoids are swollen or inflamed veins in your anus and lower rectum. These enlarged veins can cause pain, anal itching and rectal bleeding.
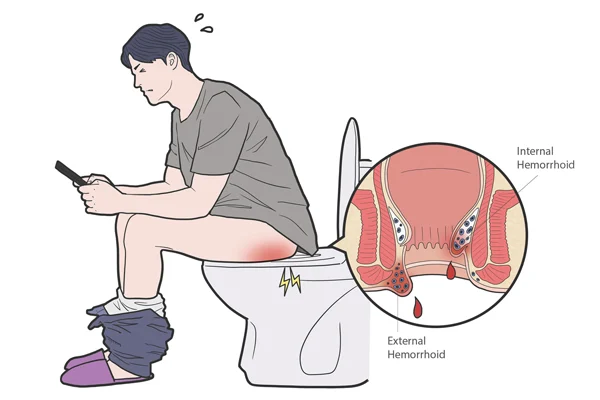
Hemorrhoids can develop inside the rectum (internal hemorrhoids) or under the skin around the anus (external hemorrhoids):
- Internal hemorrhoids are swollen veins that are located in the inside lining of the rectum. Its symptoms include bleeding after passing stool but it is usually painless. There may be a sensation of feeling soft bits of tissue protruding through the anus after defecation.
- External hemorrhoids are swollen veins located under the skin around the anus. Symptoms may include pain, bleeding, itchiness and swelling on passing stools. If the pain experienced is severe, it could mean blood clots in the vessel (thrombosis).
Signs & Symptoms of Hemorrhoids
Hemorrhoids can be uncomfortable and sometimes alarming, but knowing the common signs can help you identify the problem early. Watch out for the following symptoms:
- Painful lump or bulging tissue near your anus
- Irritation and pain around the anus
- Painful bowel movements
- Blood on your tissue after pooping
- Fecal leakage
Who Might Get Hemorrhoids
Hemorrhoids are mostly seen in adults above 30 years old and in pregnant women but even teenagers can get it.
It is associated with straining during defecation and constipation as well as situations that cause increased pressure in the haemorrhoidal veins.
Pregnant women may have this condition because of the pressure of an enlarged uterus and hormonal changes.
Your risk of getting hemorrhoids increases if you:
Tip: Prolonged sitting on the toilet even for “quick breaks” with your phone, can increase pressure on the veins in your rectum by 45%, contributing to hemorrhoids.
Try to limit your time in the bathroom and maintain healthy bowel habits.
Many people notice blood in their stool and assume it’s from hemorrhoids. What you might not see coming is the early stages of colon cancer. Keep yourself posted with what you do not know about colon cancer to prevent it from happening.
How Are Hemorrhoids Diagnosed
Hemorrhoids can be diagnosed by a doctor based on symptoms and a physical exam.
Diagnosis can also be done with:
1. Digital Rectal Exam
Your provider inserts a gloved, lubricated finger into the rectum to feel for anything unusual such as swollen veins or growths.
2. Visual inspection
Because internal hemorrhoids are often too soft to be felt during a rectal exam, your doctor might examine the lower portion of your colon and rectum with an anoscope, proctoscope or sigmoidoscope.
These tests may be uncomfortable but are not painful and can be done without anesthesia. Patients can go home the same day.
Your doctor may also recommend using colonoscopy to check your entire colon if:
- Your signs and symptoms suggest you might have another digestive system disease
- You have risk factors for colorectal cancer
- You are middle-aged and have not done a colonoscopy recently
What Can I Do About My Hemorrhoids
Some hemorrhoids symptoms often go away on their own without treatment. Symptoms like pain and bleeding may last one week or slightly longer.
You can take the following steps to reduce its symptoms:
1. Prevent Constipation
- Add more fiber in your diet (eat more fresh fruits and vegetables, take whole grain foods and less processed carbohydrates)
- Drink at least eight glasses of water per day
- Exercise regularly
- Avoid laxatives which can lead to diarrhea and worsen the hemorrhoids
2. Relieving Pain
- If you have a bath tub, it is advised to soak in a warm bath for 10 to 20 minutes a day
- If any swelling occurs, use ice packs to reduce it or sit in a warm basin of water added with salt
- Take pain-relief medications such as paracetamol, aspirin or ibuprofen to reduce the pain
Medical Treatment for Hemorrhoids
You should consult a doctor if symptoms get worse or become persistently bothersome. Seek help if the condition does not improve after a week of trying out the home remedies.
Medical treatment consists of outpatient and inpatient procedures:
- Rubber band ligation: A small rubber band placed around the base of a hemorrhoid stops the blood supply to the vein, causing the lesion to shrink.
- Hemorrhoidectomy: Surgery to remove large external hemorrhoids or prolapsed internal ones. It requires 2-4 weeks for recovery.
- Hemorrhoid stapling: A stapling instrument removes an internal hemorrhoid. Or it pulls a prolapsed internal hemorrhoid back inside the anus and holds it there.
Recurrence of Hemorrhoids
Hemorrhoids can come back, even after surgery or other medical treatments aimed at removing them.
To reduce the risk of recurrence, it’s important to address the underlying factors that contribute to hemorrhoids. This includes avoiding constipation, minimising straining during bowel movements, and making lifestyle adjustments such as increasing dietary fiber and staying hydrated.
By managing these habits, you can help prevent future flare-ups and maintain long-term relief.
Not all gut symptoms are what they seem. What feels like a minor irritation could sometimes be a sign of a more serious condition involving your colon. Learn more about common GI issues and expert guidance from Island Hospital’s Gastroenterology FAQs to protect your health.
Healthy Bowels, Healthy Life
Hemorrhoids might feel like an embarrassing inconvenience, but ignoring them can make life uncomfortable and no one should have to tiptoe around the bathroom.
Whether it’s persistent pain, bleeding, or recurring flare-ups, our Gastroenterologists at Island Hospital can help you find relief that actually lasts.
A quick consultation could be the difference between another week of discomfort and finally reclaiming your day-to-day comfort.
FAQs
How to treat hemorrhoids during pregnancy?
Hemorrhoids are common during pregnancy due to increased pressure on the pelvic veins and hormonal changes that relax blood vessels.
While they can be uncomfortable, there are safe ways to manage and relieve symptoms:
- Increase Fiber Intake: Eat plenty of fruits, vegetables, whole grains, and legumes to prevent constipation and reduce straining.
- Stay Hydrated: Drink enough water throughout the day to keep stools soft.
- Gentle Exercise: Activities like walking or prenatal yoga can improve circulation and reduce vein swelling.
- Avoid Long Periods of Sitting or Standing: Take short breaks to move around, which reduces pressure on the rectal area.
- Use Safe Topical Treatments: Pregnancy-safe creams, ointments, or sitz baths can help reduce pain, itching, and swelling.
- Practice Good Toilet Habits: Avoid straining and limit time on the toilet, including scrolling on your phone
Can hemorrhoids harm pregnancy?
Hemorrhoids during pregnancy are common, but in most cases, they do not harm the baby or affect the pregnancy.
They are primarily a source of discomfort, causing itching, pain, swelling, or occasional bleeding during bowel movements.
However, there are a few considerations:
- Severe Pain or Bleeding: Rarely, large hemorrhoids that bleed heavily may require medical attention to prevent anemia or infection.
- Discomfort During Labor: Hemorrhoids may become more swollen or painful during delivery due to pushing, but they typically do not interfere with the labor process.
- Preventing Complications: Managing constipation, avoiding straining, and using safe remedies can reduce discomfort and lower the risk of worsening hemorrhoids.
What are the risks of untreated hemorrhoids?
Most hemorrhoids are mild and can improve with lifestyle changes, but leaving them untreated can lead to persistent discomfort and potential complications:
- Chronic Pain and Itching: Untreated hemorrhoids may become increasingly painful or itchy, affecting daily activities and quality of life.
- Persistent Bleeding: Repeated rectal bleeding can sometimes lead to anemia, especially in severe or chronic cases.
- Thrombosed Hemorrhoids: External hemorrhoids can form blood clots, causing sudden, severe pain and swelling.
- Prolapse: Internal hemorrhoids may protrude outside the anus, making hygiene more difficult and increasing irritation.
- Infection: Although rare, untreated hemorrhoids can become infected, leading to redness, warmth, and pus formation.
Why did I suddenly develop hemorrhoids?
Hemorrhoids can appear suddenly, even if you’ve never experienced them before. Common triggers for sudden hemorrhoids include:
- Straining During Bowel Movements: Constipation or diarrhea can put extra pressure on the rectal area.
- Prolonged Sitting: Spending long periods on the toilet or sitting at a desk for hours can increase pressure.
- Heavy Lifting: Repeatedly lifting heavy objects can strain the rectal veins.
- Pregnancy: Hormonal changes and increased pelvic pressure can trigger sudden hemorrhoids.
- Low-Fiber Diet or Dehydration: Hard stools and constipation can contribute to sudden flare-ups.
- Lifestyle Habits: Even seemingly small habits, like spending too much time on your phone while on the toilet, can increase pressure and trigger hemorrhoids.
Does having hemorrhoids mean you’re unhealthy?
Not necessarily. Hemorrhoids are very common and affect millions of people at some point in their lives, even those who are otherwise healthy.
They are caused by increased pressure on the rectal veins, not by being “unhealthy” in general.