04 Apr A Guide to Early Detection of Stomach Cancer by Dr. Robert Ding
A Guide to Early Detection of Stomach Cancer by Dr. Robert Ding
By Island Hospital | April 4, 2025 6:51:41 PM
Medical Reviewer: Medical Officer
According to the 2022 Global Cancer Observatory, stomach cancer was the 11th most common cancer in Malaysia (1,528 new cases) and the 8th leading cause of cancer-related deaths (1,223 cases).
While not the most prevalent cancer, it continues to pose a significant health challenge. Thousands of diagnoses each year devastate individuals and families, making increased awareness, effective prevention, and early detection crucial.
Proactive gut health is crucial for overall well-being and may play a role in reducing risk. Let’s explore its importance and practical protective strategies in reducing the associated risks.
This article is based on a 2021 sharing on Stomach Cancer by Dato’ Dr Robert Ding, Island Hospital’s Consultant Gastroenterologist and Hepatologist.
Understanding Stomach Cancer
Stomach cancer, also known as gastric cancer, develops when cells in the lining of the stomach grow uncontrollably. There are different types of stomach cancer, such as:
- Adenocarcinomas (most common)
- Gastrointestinal stromal tumors (GISTs)
- Lymphomas
- Neuroendocrine tumors (including carcinoids)
- Other rare cancer types (e.g. squamous cell carcinomas, small cell carcinomas, and leiomyosarcomas)
Understanding the basic anatomy of the stomach (a muscular organ that digests food) is crucial for grasping how cancer can develop and spread.
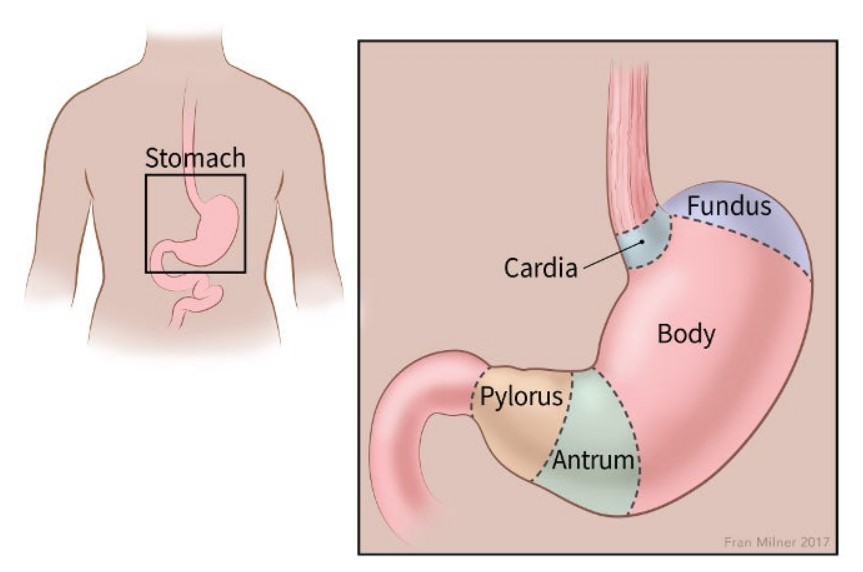
Your stomach is divided into five main sections:
- The top three (cardia, fundus, and body) are where acid, digestive enzymes, and a crucial protein (intrinsic factor, needed for B12 absorption) are produced.
- The bottom two (antrum and pylorus) handle mixing food with digestive juices and controlling its release into the small intestine.
The stomach wall itself has five layers, starting with the mucosa where most stomach cancers begin.
As cancer spreads through these layers, it becomes more advanced, impacting treatment and outlook. Nearby organs include the intestines, liver, spleen, and pancreas.
Risk Factors for Stomach Cancer
Unfortunately, there are many myths surrounding stomach cancer, and one common misconception is that it’s always hereditary.
While family history plays a role, lifestyle, and environmental factors are also significant:
- Helicobacter pylori infection
Although most individuals are asymptomatic, certain strains of the common bacteria H. pylori can cause stomach ulcers and, through chronic inflammation, increase the risk of contracting stomach cancer. - Dietary Factors
A diet high in processed meats, salty foods, smoked foods, or pickled foods increases the risk of stomach cancer due to the presence of carcinogens (e.g. N-nitroso compounds (NOCs) and polycyclic aromatic hydrocarbons (PAHs)), high salt content, and potential for H. pylori infection. - Smoking and Alcohol
Smoking and alcohol increase stomach cancer risk by directly damaging stomach cells, promoting inflammation, and potentially causing other issues like acid reflux and nutritional deficiencies. - Family History and Genetics
Having a close relative with stomach cancer increases your risk, suggesting a possible genetic predisposition. - Age and Gender
In Malaysia, stomach cancer is diagnosed more frequently in men of Chinese ethnicity compared to other groups. - Previous Stomach Conditions
Previous conditions like gastritis and stomach ulcers can also increase this risk. - Other Factors
Less common factors include certain occupations (e.g., coal mining), pernicious anemia, and previous stomach surgery.
It’s important to understand your individual risk. While some factors are unmodifiable (like age or genetics), many are within your control.
Talk to your doctor about your risk profile. They can help you assess your risk level (low, moderate, or high) and recommend appropriate screening or preventive measures.
Digestive problems can be concerning, but they aren’t always a sign of stomach cancer. Discover 8 common conditions, besides stomach cancer, that could be affecting your gut health.
Prevention: Taking Control of Your Gut Health
Gut health is crucial, and prevention is paramount. Here’s how you can take charge and start protecting your gut today with two main categories:
1. Primary Prevention: Preventing Stomach Cancer Before It Starts
- Dietary Strategies (Actionable Advice)
A diet rich in whole foods, fruits, and vegetables is a cornerstone of gut health. Focus on incorporating these into your daily meals:
Types of Food Dietary Functions Fruits and Vegetables - Avocados: Rich in healthy fats and fiber.
- Blueberries: Packed with antioxidants.
- Turmeric: Contains curcumin, a compound with anti-inflammatory properties.
- Garlic: May have anti-cancer properties.
- Tomatoes: A good source of lycopene, an antioxidant.
- Strawberries & Grapes: Provide vitamins and antioxidants.
- Broccoli & Cabbage: Cruciferous vegetables linked to reduced cancer risk.
- Citrus Fruits: Excellent source of Vitamin C.
Whole Grains - Choose whole-wheat bread, brown rice, quinoa, and oats over refined grains.
- Promotes healthy digestion, protecting cells from damage, and supporting a balanced gut microbiome.
Beverages - Opt for green tea instead of other tea options.
- Green tea polyphenols increase the antimutagenic activity of green tea, potentially inhibiting cancer.
Foods to Limit or Avoid for Stomach Health:- Processed Meats (e.g., bacon, sausage, ham): These contain carcinogens formed during processing.
- Salty Foods: High salt intake can damage the stomach lining.
- Smoked & Preserved Foods (e.g., pickled vegetables): These may contain carcinogens. Pickled foods, in particular, have been linked to increased stomach cancer risk in some populations. This is likely due to the high salt content and the fermentation process.
2. Lifestyle Modification
- Smoking Cessation: Quitting smoking is one of the most important steps you can take as it damages the stomach lining and increases the risk of stomach cancer and also ulcers.
Numerous resources are available to help you quit, as seen on Nicorette. - Moderate Alcohol Consumption
Excessive alcohol intake can irritate the stomach lining and contribute to various digestive issues. If you choose to drink alcohol, do so in moderation.
Generally, this means no more than one standard drink per day for women and no more than two standard drinks per day for men. - Healthy Weight
A healthy weight, achieved through a balanced diet and regular physical activity, is vital to digestive health. Excess weight can contribute to conditions like acid reflux and hiatal hernias.
Aim for at least 150 minutes of moderate-intensity exercise per week! Consult with a healthcare professional or registered dietitian for personalized advice on diet and exercise. - Stress Management
Chronic stress can negatively impact gut health. Aside from a healthy mind, stress management techniques such as mindfulness, yoga, meditation, or time in nature also help improve your gut health. - Avoid NSAIDs
NSAIDs (like ibuprofen and naproxen) can irritate the stomach and increase the risk of ulcers and bleeding, especially with long-term use.
If you regularly use NSAIDs, talk to your doctor about pain management alternatives and ways to minimize stomach problems. Never exceed the recommended dosage.
3. Secondary Prevention: Detecting and Addressing Issues Early
Secondary prevention focuses on early detection and treatment of conditions that can increase the risk of stomach cancer. Here are some of them:
- Managing H. pylori
H. pylori is a Group 1 carcinogen, meaning it is a known cause of cancer. It’s a common bacterium that can cause inflammation in the stomach lining, increasing the risk of ulcers and stomach cancer.
This makes testing for H. pylori important especially if you have a history of stomach ulcers or other risk factors. Treatment typically involves a course of antibiotics. Following the prescribed regimen is crucial for eradicating the bacteria. - Surveillance of Precancerous Lesions
Regular checkups and screenings can help detect precancerous changes in the stomach lining. This may involve:
(a) Endoscopy: A procedure where a thin tube with a camera is inserted into the stomach to visualize the lining. Biopsies can be taken for further examination.
(b) Upper GI Series: An X-ray of the esophagus, stomach, and duodenum.
Are mindless snacking habits contributing to unwanted weight gain? This article on healthy snacking provides insights and actionable steps to help you regain control over your snacking and manage your weight effectively.
Early Detection
1. Recognizing the Signs and Symptoms
Early detection is critical for successful treatment. Be aware of these potential warning signs and when to see a doctor:
- Bloating or feeling full after eating very little
- Blood in stool or vomit (this is a serious sign and requires immediate medical attention.)
- Difficulty swallowing
- Loss of appetite
- Nausea and vomiting
- Persistent abdominal pain
- Unexplained weight loss
It’s crucial to differentiate between occasional indigestion and concerning symptoms. Occasional heartburn or indigestion is usually not a cause for alarm.
However, persistent symptoms, especially any of those listed above, warrant a visit to your doctor. Don’t delay seeking medical advice.
2. Screening for High-Risk Individuals
Even without experiencing any symptoms, individuals with certain risk factors should consider screening for stomach cancer such as:
- A first-degree relative (parent, sibling, child) with stomach cancer.
- Having chronic gastritis of the stomach lining.
- Having Helicobacter Pylori Infection.
- Intestinal Metaplasia (This condition, where stomach cells change to resemble intestinal cells, is a precancerous change.)
- Inherited conditions like Lynch syndrome, familial adenomatous polyposis, and hereditary diffuse gastric cancer.
- Pernicious anemia
- Previous stomach surgery.
3. Diagnostic Procedures
The primary screening method for stomach cancer is upper endoscopy.
This procedure involves inserting a thin, flexible tube with a camera into the stomach to visualize the lining and take tissue samples (biopsies) for examination under a microscope.
While upper endoscopy is the primary diagnostic tool, other tests may play a supporting role such as:
- Serological Screening (Blood Tests)
Blood tests can sometimes detect certain tumor markers associated with stomach cancer. However, these markers are not specific enough for reliable widespread screening and are more often used to monitor treatment progress or recurrence. - Imaging Techniques (CT/MRI Scans)
CT and MRI scans are valuable tools for determining the extent (stage) of stomach cancer once it has been diagnosed. They are not typically used for initial screening due to their limited ability to detect early-stage cancers and higher cost.
Your Gut Health Matters!
A proactive approach to early screening and a healthy lifestyle is your best defence against stomach cancer.
Learn more about the different stomach cancer screening methods with Island Hospital’s clinical oncology department and digestive centre.
Ready to discuss your gut health with an expert? Book an online appointment in just 3 easy steps with one of our experienced gastroenterologists today.
FAQ
1. How do I check myself for stomach cancer?
It’s important to understand that you cannot self-check for stomach cancer in the way you might check for a lump in your breast or on your skin. Stomach cancer develops inside the body and often doesn’t cause noticeable symptoms in its early stages.
Instead of self-checking,focus on understanding your risk factors, recognizing potential symptoms, and consulting your doctor for appropriate screening and advice.
2. How can stomach cancer be detected early?
Early stomach cancer detection relies on understanding risk factors and recognizing potential symptoms like persistent abdominal pain or unexplained weight loss. Screening, primarily through endoscopy, is recommended for high-risk individuals.
Diagnosis requires medical evaluation and procedures like biopsies and imaging tests, emphasizing the importance of consulting a doctor for any concerning symptoms.
3. Does cancer make you hungry all the time?
Cancer does not necessarily make you hungry all the time. In fact, one of the potential symptoms of stomach cancer can be a loss of appetite or feeling full after eating only a small amount. This can sometimes lead to weight loss.