08 Apr Is it Just a Heavy Period? 5 Uncommon Signs of Endometriosis
Is it Just a Heavy Period? 5 Uncommon Signs of Endometriosis
By Island Hospital | 8 April 2026. 10:00:00 AM
Endometriosis can start as more than just “bad period pain.” It might feel like chronic pelvic pain, sharp discomfort during sex, heavy or unpredictable bleeding, or constant fatigue that disrupts work and daily life.
This condition affects an estimated 1 in 10 women worldwide.
Despite being common, diagnosis often takes years, leaving many to cope with pain and emotional stress without answers.
Let’s find out how endometriosis can impact your body and its hidden signs to look out for.
What Is Endometriosis?
Endometriosis is a chronic condition that occurs when tissue similar to the lining of the uterus grows outside the womb.
This misplaced tissue can grow on the ovaries, fallopian tubes, bowel, bladder, or the lining of the pelvis. Like the uterine lining, it responds to hormonal changes during the menstrual cycle, thickening and breaking down each month.
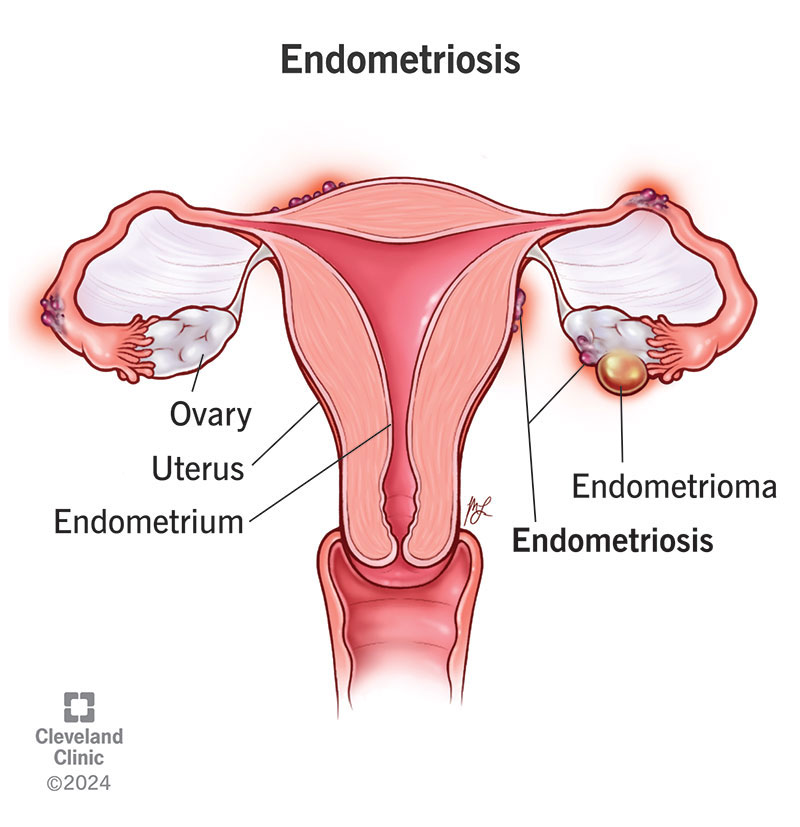
However, because it has nowhere to go, the blood and tissue become trapped inside the body. Over time, this can lead to inflammation, scar tissue (adhesions), and sometimes cysts.
The resulting pain is often caused by inflammation, irritation of nearby nerves, and organs sticking together due to these adhesions.
Symptoms of Endometriosis
Endometriosis symptoms can vary widely. Some people experience severe, life-disrupting pain, while others may have subtle or even no noticeable symptoms.
1. Most Common Symptoms
The most recognised signs of endometriosis include:
- Severe menstrual cramps that feel worse than typical period pain
- Chronic pelvic pain that may persist outside of menstruation
- Pain during or after sex (deep pelvic pain)
- Heavy, prolonged, or irregular periods
- Lower back pain, especially around the menstrual cycle
2. Less Recognised Symptoms
Endometriosis can also affect other organs in the pelvis, leading to symptoms that are often mistaken for digestive or urinary conditions:
- Bloating (sometimes called “endo belly”), diarrhea, or constipation
- Painful bowel movements or urination, particularly during periods
- Persistent fatigue and low energy
- Nausea
- Migraines or headaches linked to the menstrual cycle
3. Silent Endometriosis
Not everyone experiences obvious symptoms. Some people have little to no pain, and endometriosis is only discovered during fertility investigations or unrelated pelvic surgery.
This variation in symptoms is one reason the condition can be difficult to diagnose.
Causes of Endometriosis
The exact cause is unknown, but several factors may contribute:
- Retrograde menstruation: menstrual blood flows backward into the pelvis
- Genetics: family history increases risk
- Hormonal factors: estrogen promotes tissue growth
- Immune dysfunction: the body fails to clear misplaced cells
Most experts believe it results from a combination of these factors.
If you notice any changes to your body or the above underlying symptoms, it is time to get them checked.
Island Hospital’s Women’s Health Screening Package is designed to provide a comprehensive look at your pelvic health with the care and sensitivity you deserve.
Minimally invasive laparoscopic surgery allows doctors to accurately diagnose and treat conditions like endometriosis with precision and faster recovery. Check out this article on “What to Expect During a Laparoscopic Surgery”.
How Does Endometriosis Affect Your Daily Life?
Endometriosis affects far more than just your physical health because it is often an unpredictable condition.
It can ripple into every area of life such as by impacting emotional wellbeing, career stability, relationships, and your overall quality of life.
1. Mental & Emotional Impact
Living with ongoing pain and uncertainty can take a serious emotional toll. Many individuals experience:
- Anxiety and depression
- Emotional exhaustion from managing persistent symptoms
- Reduced overall quality of life
- Feeling misunderstood, dismissed, or not taken seriously
The unpredictability of flare-ups, not knowing when pain will strike or how severe it will be can also create constant stress and a sense of loss of control.
2. Work and Career Challenges
Endometriosis can significantly impact professional life. Severe pain, fatigue, and medical appointments may lead to:
- Frequent sick leave
- Reduced concentration and productivity
- Difficulty maintaining full-time or demanding schedule
- Career slowdowns or interruptions
Because menstrual health is still stigmatised in many workplaces, some individuals feel uncomfortable disclosing their condition, adding another layer of stress.
3. Relationships & Intimacy
This condition can also affect personal relationships. Pain during intimacy (dyspareunia), fertility concerns, and emotional strain may create distance between partners.
Some individuals withdraw socially due to fatigue or fear of flare-ups, making communication and support even more important.
Is Endometriosis & Adenomyosis the Same?
Although these conditions can share similar symptoms, they are not the same. The key difference lies in where the tissue grows and how it affects the body.
Let’s take a look at them:
| Medical Condition | What Happens | Common Symptoms |
|---|---|---|
| Endometriosis | Tissue similar to the uterine lining grows outside the uterus (e.g., ovaries, fallopian tubes, pelvic lining). | Chronic pelvic pain, painful periods, pain during sex, infertility, bowel or bladder symptoms. |
| Adenomyosis | Tissue similar to the uterine lining grows within the muscular wall of the uterus. | Heavy or prolonged menstrual bleeding, severe cramping, enlarged or tender uterus, pelvic pressure. |
| PCOS | A hormonal disorder that affects how the ovaries function and ovulate. | Irregular or absent periods, acne, weight gain, excess facial/body hair, fertility challenges. |
While endometriosis and adenomyosis are related to abnormal tissue growth, PCOS is primarily a hormonal condition.
As symptoms to these medical conditions tend to overlap especially around pain and fertility, proper medical evaluation from a skilled gynaecologist is important for an accurate diagnosis.
Endometriosis Diagnosis
Diagnosing endometriosis usually involves several steps, as there is no single simple test that can confirm it immediately.
Step 1: Medical History & Symptom Review
Your doctor will ask detailed questions about your menstrual cycle, pain patterns, digestive or urinary symptoms, and fertility concerns. This helps identify possible signs of endometriosis early.
Step 2: Pelvic Examination
During a physical exam, the doctor checks for tenderness, nodules, or abnormalities in the pelvic area that may suggest endometrial tissue outside the uterus.
Step 3: Imaging Tests (Ultrasound or MRI)
Ultrasound or MRI scans can help detect cysts (endometriomas) or signs of deep endometriosis. Keep in mind that small or superficial lesions may not always be visible on imaging.
Step 4: Laparoscopy Surgery (Gold Standard)
If endometriosis is strongly suspected, a laparoscopy may be performed. This allows the doctor to directly view, biopsy, or remove endometrial tissue, providing a definitive diagnosis.
Since early or small lesions can be hard to spot, diagnosis may take time. Going through these steps helps ensure a thorough evaluation and the most effective treatment plan for you.
What Treatments Are Available for Endometriosis?
Endometriosis treatment depends on symptom severity, desire for fertility, and overall health. The approaches often combine medical, surgical, and lifestyle strategies.
Here’s a breakdown of what they are and their pros and cons:
| Treatment Type | What It Involves | Pros | Cons |
|---|---|---|---|
| Pain Management | NSAIDs (e.g., ibuprofen), heat therapy, physical therapy | Accessible, non-invasive, helps relieve pain | Does not treat the underlying disease; symptoms may persist |
| Hormone Therapy | Birth control pills, hormonal IUDs, GnRH medications | Can slow disease progression, reduces pain | Possible side effects; symptoms may return if treatment stops |
| Surgical Treatment | Laparoscopic removal of endometrial lesions | Can significantly reduce pain, improve fertility | Endometriosis may recur; carries surgical risks |
| Lifestyle Management | Anti-inflammatory diet, stress reduction, regular exercise | Supports overall wellbeing, complements medical treatments | Cannot replace medical or surgical intervention for severe cases |
How to Manage Endometriosis in Daily Life
Living with endometriosis can be challenging, but practical daily strategies can help reduce symptoms and improve quality of life:
1. Diet Approaches
- Focus on healthy diet and anti-inflammatory foods (fruits, vegetables, leafy greens)
- Include omega-3 rich foods (salmon, chia seeds, walnuts)
- Limit processed sugars and highly processed foods
2. Exercise
- Gentle activities like yoga, walking, or swimming
- Improves circulation, reduces stress, and increases pain tolerance
- Exercises that ease endometriosis
3. Stress Reduction & Emotional Support
- Mindfulness practices, meditation, or breathing exercises
- Therapy or support groups for emotional wellbeing
- Adequate sleep and relaxation routines
4. Pain Coping Strategies
- Heat therapy for cramping or pelvic pain
- Tracking symptom patterns to identify triggers
- Relaxation techniques to help manage flare-ups
Combining these strategies with medical or surgical treatments often gives the best results for managing symptoms and improving daily life.
Aside from endometriosis, uterine fibroids can also cause pelvic pressure, heavy periods, and urinary symptoms. Learn about effective treatment options in our guide to managing fibroids.
When Should I Seek Medical Help
Consider speaking to a healthcare professional if you experience:
If your symptoms feel persistent, severe, or different from what others describe as “normal,” it’s worth seeking medical advice. You deserve to have your pain taken seriously.
Questions to ask your doctor:
- Could my symptoms indicate endometriosis?
- What tests do I need?
- What treatment options fit my goals?
Take Back Control from Endometriosis
Living with endometriosis can be exhausting. The pain, fatigue, and uncertainty can affect every part of your life. But you don’t have to face it alone.
With the right combination of treatments, lifestyle strategies, and support, many people find relief and regain control over their daily lives.
At Island Hospital, our compassionate Obstetrics & Gynaecology team listens, understands, and works with you to create a treatment plan that fits your needs. From managing pain to supporting fertility and overall wellbeing, we’re here to help you feel heard and cared for every step of the way.
Reach out today and take the first step toward living life on your terms again.
FAQs
Why does it take years to diagnose endometriosis?
Endometriosis is one of the most frequently misdiagnosed or overlooked gynecological conditions. On average, many people wait years before receiving a clear diagnosis.
Several factors contribute to this delay such as symptoms that are often dismissed as “normal period pain,” especially in teenagers and young adults.
The condition also presents differently from person to person whereby some experience severe pain, while others have milder or atypical symptoms which makes diagnosis harder.
Consequently, awareness and training can vary among healthcare providers, and standard imaging tests such as ultrasounds do not always detect early or smaller lesions. In many cases, a definitive diagnosis requires laparoscopic surgery, which may not be immediately recommended.
As a result, many people spend years seeking answers, trying different treatments, and coping with worsening symptoms before finally being diagnosed.
Does endometriosis get worse with age?
Symptoms often improve after menopause when hormone levels drop, but this is not the same for everyone. Some people continue to experience pelvic pain or other symptoms even after their periods stop.
Age alone doesn’t determine how severe symptoms are, as severity varies widely. Therefore, early recognition and management are key to reducing long-term impact.
Is endometriosis hereditary?
Endometriosis can run in families, meaning having a close relative with the condition increases your risk. However, it doesn’t guarantee you will develop it.
Genetics is just one factor as hormonal, environmental, and immune system factors also play a role. Being aware of family history can help with earlier recognition and timely management.
Can teenagers have endometriosis?
Yes, endometriosis can start soon after the first period, even in teenagers. Symptoms like severe cramps, heavy bleeding, or pelvic pain are sometimes mistaken for normal menstrual discomfort.
Early awareness and proper evaluation can help prevent years of untreated pain. Teenagers and their caregivers should seek medical advice if symptoms are severe or worsening.
Does pregnancy cure endometriosis?
No, pregnancy does not cure endometriosis. Some people may notice temporary relief from symptoms due to hormonal changes during pregnancy.
However, symptoms often return after childbirth or when hormone levels normalise. Pregnancy should not be viewed as a treatment strategy, and proper medical management remains important.