06 Apr Finding the Right Overactive Bladder Treatment and Options That Actually Work
Finding the Right Overactive Bladder Treatment and Options That Actually Work
By Island Hospital | 6 April 2026. 10:00:00 AM
Medical Reviewer:
If you have an overactive bladder (OAB), even simple plans can start to revolve around one question: “Where’s the nearest restroom?”
A long drive, a flight, a movie, or even a short meeting can feel stressful when you’re constantly worried about sudden urges, frequent bathroom trips, or possible leaks.
Many people living with OAB find themselves mapping out toilets before travelling, limiting how much they drink, or avoiding activities they once enjoyed which can take a real toll on confidence, sleep, and daily life.
The good news is that while OAB can be frustrating and sometimes embarrassing, it’s also highly treatable and manageable with the right support, lifestyle strategies, and medical care you need.
What Is an Overactive Bladder?
OAB is unlike a single disease but more of a group of symptoms that happen when your bladder muscle squeezes (contracts) suddenly, even when your bladder isn’t full.
This creates a strong, hard-to-control urge to urinate that can come on very quickly.
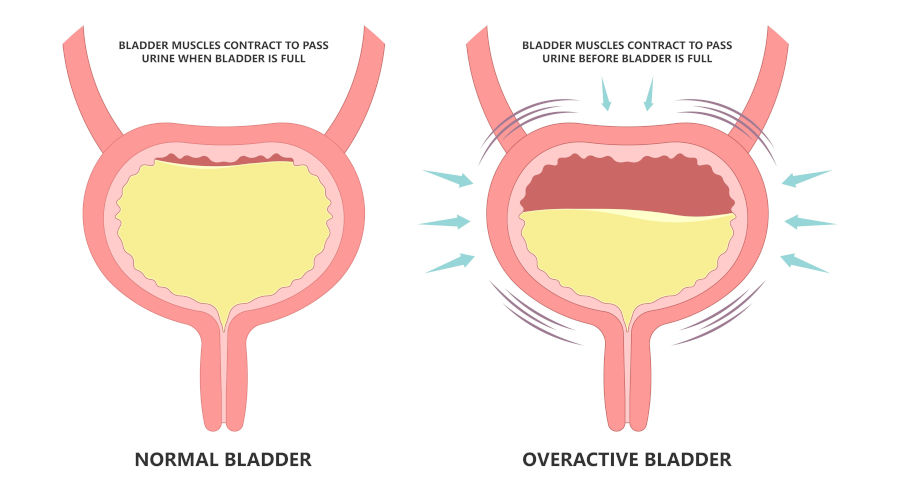
It is mainly identified by these noting symptoms:
These symptoms can do more than just inconvenience you as they can affect sleep quality, work focus, travel plans, and social confidence, making everyday activities feel stressful or unpredictable.
What Causes An Overactive Bladder
OAB happens when the bladder muscles become overly sensitive or contract at the wrong time even when your bladder isn’t full. This creates a sudden urge to urinate that can be hard to control.
Some factors that can contribute to OAB are:
1. Nerve & Muscle Dysfunction
Your bladder depends on a complex system of nerves and muscles to store and release urine at the right time. OAB can occur when these signals become disrupted, causing the bladder muscle to squeeze unexpectedly.
2. Medical Conditions Linked to OAB
Certain health conditions can increase the risk of developing OAB by affecting nerves, muscles, or bladder control. These include:
- Diabetes
- Stroke
- Parkinson’s disease
- Spinal cord injuries
- Enlarged prostate (in men)
3. Lifestyle Triggers
Some everyday habits can irritate the bladder or worsen symptoms, such as:
- Drinking caffeine or alcohol
- Consuming too much fluid in a short time
- Smoking
- Chronic constipation
- Being overweight or obese
3. Age and Gender Factors
OAB becomes more common as people get older, but it is not a normal part of aging. Hormonal changes after menopause can increase risk in women, while in men, symptoms are often linked to prostate enlargement.
How Doctors Diagnose Overactive Bladder
Diagnosing OAB mainly involves ruling out other causes of urinary symptoms and understanding your bladder patterns.
Standard clinical guidelines encompass doctors following a step-by-step evaluation process:
1. Medical History & Symptom Review
Your doctor will ask about:
- How often you urinate during the day and night
- Fluid intake and caffeine or alcohol consumption
- Episodes of urine leakage
- Lifestyle habits that may affect bladder function
2. Bladder Diary
You may be asked to keep a bladder diary for several days. Recording urination times, amounts, and urgency helps identify patterns and triggers.
3. Urine Tests
Simple urine tests can rule out infections, blood in the urine (hematuria), or diabetes, which can cause similar symptoms.
4. Specialised Testing
In more complex cases, doctors may use advanced tests such as:
- Urodynamic testing: measures how well the bladder stores and releases urine
- Bladder scans: check for residual urine or abnormalities
- Cystoscopy: a camera examines the inside of the bladder for structural issues
Our urologist specialists will ensure an accurate diagnosis to help you manage your OAB symptoms with a personalised treatment plan for you.
Specialised bladder tests can help detect overactive bladder early and guide treatment. Explore how Island Hospital’s advanced health screenings can support your bladder health in our article on Health Screening Services.
Best Treatments for Overactive Bladder
Treating OAB usually follows a stepwise approach, starting with the least invasive options. Here’s a structured “treatment ladder” to help our patients manage symptoms effectively:
1. First-Line Treatments: Lifestyle & Behavioral Therapy
These non-invasive strategies are often the first and most effective step.
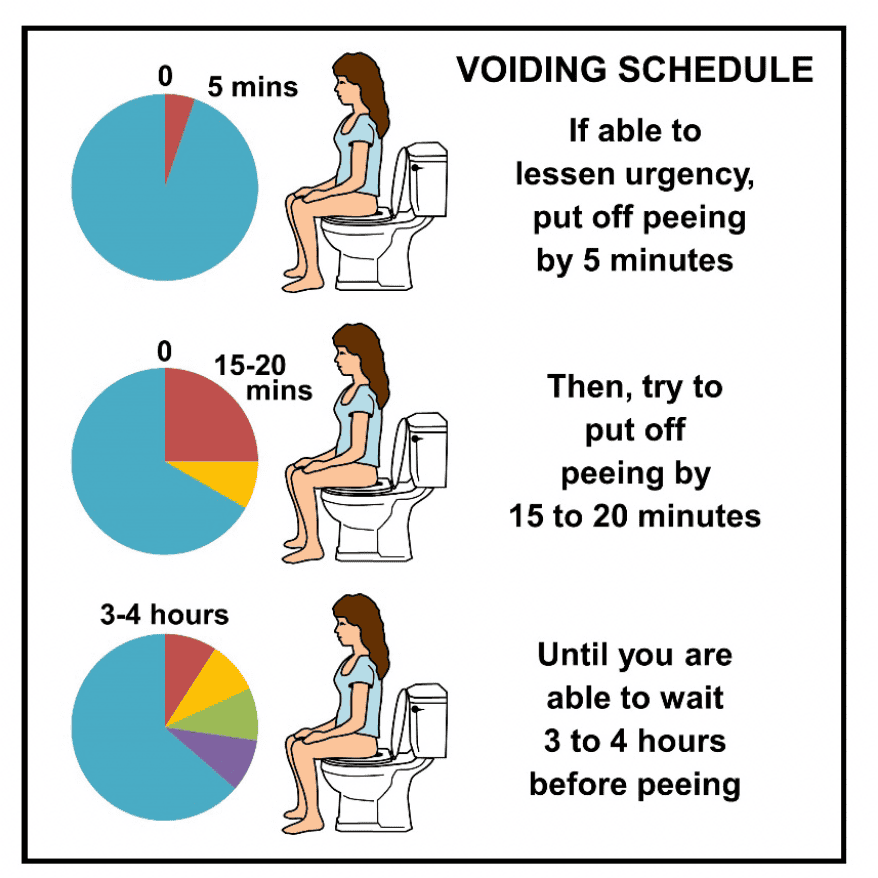
- Bladder Training
Bladder training involves following a planned voiding schedule and gradually delaying urination to increase your urine capacity in the long run.
- Pelvic Floor Exercises (Kegels)
Kegel exercises help strengthen the pelvic floor muscles that support the bladder and control urine flow. - Fluid Management
Paying attention to what, when, and how much you drink can help reduce bladder irritation and sudden urges.
Spacing fluids throughout the day, limiting caffeine and alcohol, and avoiding large amounts of liquid before bedtime can help ease urgency, frequency, and nighttime bathroom trips. - Maintain a healthy weight
Carrying excess weight can put added pressure on the bladder and surrounding pelvic muscles, which may worsen urgency, frequency, and leakage.
Maintaining a healthy weight through balanced nutrition and regular physical activity can help reduce this pressure and improve bladder control over time.
2. Medications for Overactive Bladder
If lifestyle changes alone do not provide enough relief, doctors may prescribe medications to reduce your symptoms. The following medicines work by calming or relaxing the bladder muscles:
- Anticholinergics
These medications help reduce sudden bladder muscle spasms, making it easier to control the urge to urinate.
They are commonly used but may cause side effects such as dry mouth, constipation, or blurred vision in some people.
- Beta-3 Agonists
These drugs work by relaxing the bladder muscle, allowing it to hold more urine and reducing the feeling of urgency.
They are generally better tolerated and tend to have fewer bothersome side effects compared to anticholinergics.
Both medication types help manage overactive bladder symptoms, but they work in different ways and have different side-effect profiles. Let’s take a look at them:
| Feature | Anticholinergics | Beta-3 Agonists |
|---|---|---|
| How they work | Calm bladder muscle spasms by blocking nerve signals | Relax the bladder muscle so it can store more urine |
| Main benefit | Reduce urgency, frequency, and leakage | Reduce urgency and increase bladder capacity |
| Common side effects | Dry mouth, constipation, blurred vision | Usually mild; may include headache or slight increase in blood pressure |
| Tolerance | Some people stop due to side effects | Generally better tolerated long-term |
| Who they’re often used for | Typically first medication tried | Often used if side effects occur or additional control is needed |
Your doctor will choose between these options based on your symptom severity, medical history, and how well you tolerate side effects. In some cases, both types may even be combined for better symptom control.
3. Advanced Treatments for Severe OAB
For persistent or severe cases, more specialised therapies may be considered.
- Bladder Botox Injections
Temporarily relax bladder muscles to reduce urgency and leakage. - Nerve Stimulation Therapy
Devices help regulate bladder nerve signals for better control. - Surgery
Rarely needed but may be an option in severe, treatment-resistant cases.
Starting with simple lifestyle changes and moving to more advanced therapies when needed can help you regain control, reduce symptoms, and improve your overall quality of life.
How Overactive Bladder Affects Your Daily Life
Overactive bladder is more than just a physical condition as it can affect your emotional wellbeing, confidence, and everyday routines.
Constantly needing to stay close to a restroom or worrying about sudden urges can make daily activities feel stressful, limiting, and unpredictable.
Common ways OAB can affect daily life include:
- Sleep disruption
Frequent nighttime urination can lead to poor sleep and daytime fatigue. - Social anxiety
Fear of urgency or leaks may cause embarrassment or worry in public settings. - Reduced work productivity
Frequent bathroom trips and interrupted focus can affect performance. - Avoidance of travel or outings
Many patients with OAB tend to plan activities around restroom access or avoid them altogether.
Recognising these impacts is important, as addressing both the physical symptoms and emotional challenges plays a key role in successful treatment and long-term symptom control.
When Should You See A Doctor
It’s important to seek medical advice if you notice urinary symptoms that are sudden, persistent, or worsening as early evaluation can help identify the cause and prevent further complications.
You should see a doctor if you experience:
- Sudden onset of urinary symptoms
- Blood in your urine
- Pain or burning when urinating
- Frequent nighttime urination that disrupts sleep
- Ongoing urine leakage
These symptoms may not always be due to overactive bladder and could signal other medical conditions such as kidney problems that require prompt diagnosis and treatment.
Kidney stones can irritate the bladder and worsen symptoms like urgency and frequent urination. Learn about your treatment options in our guide: 4 Effective Treatment Methods to Remove Kidney Stones.
Bid Goodbye to Urgency and Leakage
OAB is a common condition, but it does not dictate your life or take away your confidence and happiness. With the right combination of lifestyle strategies, bladder training, exercises, medications, and medical support, most people can manage their symptoms effectively.
Recognising OAB early and seeking guidance from Island Hospital can help you regain control, enjoy daily activities, and live life on your terms.
Our experienced Urology specialists will work closely with you to help you manage your symptoms effectively.
Schedule an appointment with us today if you face any OAB symptoms.
FAQs
Is overactive bladder curable?
OAB isn’t always completely curable, but the good news is that most people can manage their symptoms effectively.
With a combination of lifestyle changes, bladder training exercises, pelvic floor strengthening, medications, and, in some cases, advanced therapies, many individuals experience significant improvement in urgency, frequency, and incontinence.
Early intervention and working closely with a healthcare professional can make daily life much more comfortable and help prevent symptoms from worsening over time.
Can OAB go away on its own?
In some mild cases, OAB symptoms may improve on their own, especially when combined with simple strategies like bladder training, timed voiding, and adopting healthy lifestyle habits.
However, for many people, symptoms persist or even worsen over time, making medical evaluation important.
What foods or drinks make OAB worse?
Certain foods and beverages can irritate the bladder and make OAB symptoms more noticeable. These include:
- Caffeine (found in coffee, tea, chocolate, and some sodas) can stimulate the bladder, increasing urgency and frequency of urination.
- Alcohol acts as a diuretic, meaning it increases urine production, which can worsen both daytime and nighttime trips to the bathroom.
- Spicy foods may irritate the bladder lining, triggering urgency or discomfort in sensitive individuals.
- Acidic fruits such as oranges, grapefruits, and tomatoes can also irritate the bladder, sometimes leading to stronger urges or leakage.
Therefore, identifying and moderating these triggers will keep the intensity and frequency of your symptoms at bay.
Is OAB the same as urinary incontinence?
No, OAB and urinary incontinence are not the same, though they are related.
| Feature | Overactive Bladder (OAB) | Urinary Incontinence |
|---|---|---|
| Definition | A syndrome characterised by sudden urgency, frequent urination, and sometimes nighttime urination (nocturia) | Accidental or involuntary leakage of urine |
| Core Symptoms | Urgency, frequency, nocturia; may include leakage | Leakage of urine; may or may not include urgency or frequency |
| Relation | OAB can cause urinary incontinence, but not everyone with OAB leaks urine | Can be a symptom of OAB, but also occurs from other causes (e.g., stress, pregnancy, prostate issues) |
| Affected Areas | Bladder muscle and nerve signaling | Urinary sphincter, bladder, or pelvic floor function |
| Treatment Focus | Managing bladder overactivity (lifestyle changes, bladder training, medication) | Addressing cause of leakage (can include pelvic floor exercises, surgery, or medications) |
| Typical Patient Experience | Frequent urges, sleep disruption, need to plan bathroom trips | Embarrassment or inconvenience due to leakage, may occur during physical activity, coughing, or sneezing |
In other words, you can have OAB with urgency and frequency without any leakage, and conversely, urinary incontinence can occur due to other causes unrelated to OAB.
Understanding this distinction is important for diagnosis and choosing the most effective treatment plan.
Can OAB be caused by stress?
Yes, stress can contribute to OAB, though it’s usually not the sole cause. Emotional stress and anxiety can heighten bladder sensitivity and trigger sudden urges to urinate.
Stress may also worsen existing OAB symptoms which makes them more noticeable.
Managing stress through relaxation techniques, mindfulness, or counseling, alongside standard OAB treatments, can help reduce symptom flare-ups and improve overall bladder control.